Take a quick fun-quiz and test your kidney health knowledge!
The main job of your kidneys is to remove toxins and excess water from your blood.
Kidneys also help to control your blood pressure, to produce red blood cells and to keep your bones healthy.
Each roughly the size of your fist, kidneys are located deep in the abdomen, beneath the rib cage.
Your kidneys control blood stream levels of many minerals and molecules including sodium and potassium, and help to control blood acidity. Every day your kidneys carefully control the salt and water in your body so that your blood pressure remains the same.
Your Kidneys:
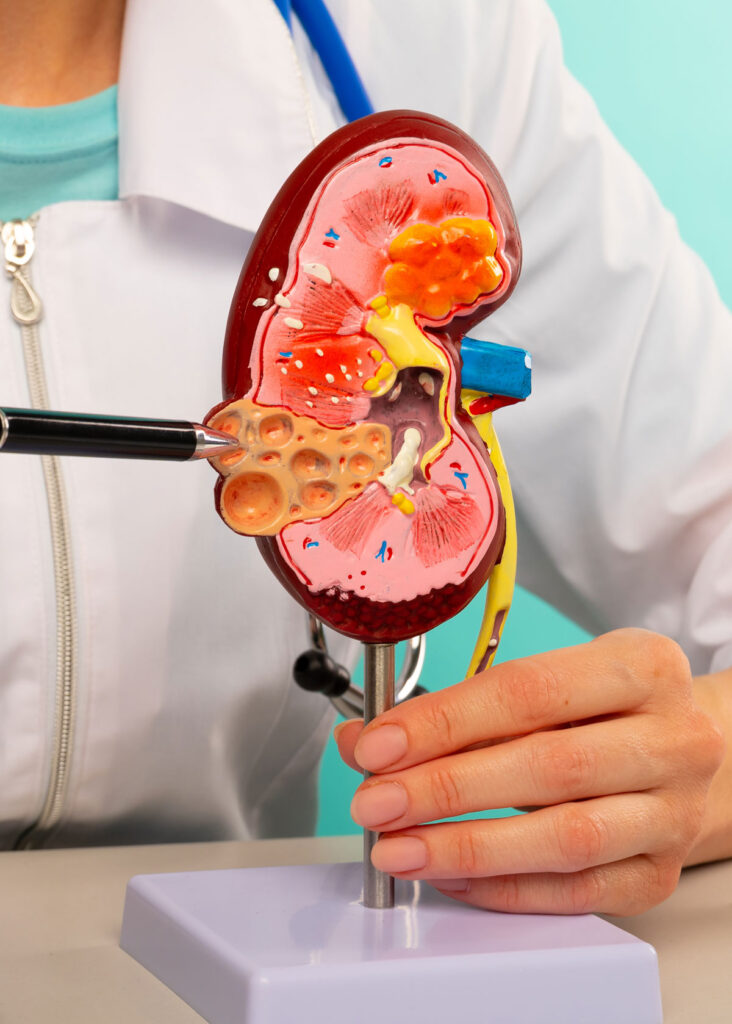
The majority of people are born with two kidneys, each made out of a million tiny units, known as nephrons. When nephrons are damaged, they stop functioning, placing added strain on the remaining healthy nephrons to sustain normal kidney function. However, if the damage continues, the remaining healthy nephrons become insufficient to maintain kidney function.
This progressive loss in kidney function over a span of months or years is called Chronic kidney disease (CKD). CKD is extremely common, with 1 in 10 of the adult population having some form of kidney damage, and every year millions die prematurely of complications related to CKD.
Most people have no symptoms until CKD is advanced. Signs of advancing CKD include:
Note: Often doctors cannot determine the root cause of CKD.
Since CKD can have no signs or symptoms, blood and urine tests are two tests to check for kidney disease. The early detection of failing kidney function is crucial because it allows proper treatment before kidney damage or deterioration manifests itself through other complications.
Simple laboratory tests are done on small amounts of blood to measure creatinine and estimate Glomerular Filtration Rate (eGFR) and on urine to measure creatinine and protein (for example albumin, light chain protein) excretion.
There are five stages of CKD based on GFR levels. When individuals reach Stage 5 and develops uremic symptoms, it is known as End-Stage-Kidney-Disease (ESKD), which requires regular dialysis treatment or a kidney transplant to survive.
| Stage | Description | eGFR Level |
| Normal Kidney Function | Healthy Kidneys | 90mL/min or more |
| Stage 1 | Kidney damage with normal or high GFR | 90ml/min or more |
| Stage 2 | Kidney damage and mild decrease in GFR | 60 to 89mL/min |
| Stage 3 | Moderate decrease in GFR | 30 to 59mL/min |
| Stage 4 | Severe decrease in GFR | 15 to 29 mL/min |
| Stage 5 (ESKD) | Established kidney failure | Less than 15mL/min or on dialysis |
Source: “KDIGO 2023 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease”.
The majority of individuals with early stages of CKD go undiagnosed. On WKD, we are calling on everyone to check if they are at risk for kidney disease and encouraging people with any risk factors to take a simple kidney function test.
While there is no cure for CKD, complications can be prevented and progression be slowed down or halted with proper treatment. It should include:
For those facing ESKD, long-term dialysis treatment or kidney transplantation is needed to remove wastes and excess fluid from the blood. Dialysis and kidney transplantation are known as kidney replacement therapies (KRT) because they attempt to “replace” the normal functioning kidneys.
Read more about:
The growing prevalence of kidney disease is placing an overwhelming financial burden on healthcare systems worldwide. While in low and middle-income countries long-term dialysis is unaffordable for the majority of patients, it is becoming increasingly inaccessible in high-income countries too.
In developed countries, ESKD is a major cost driver for patients, families and taxpayers due to the high costs of dialysis or kidney transplantation.
Developing countries, with a combined population of over 600 million people, cannot afford kidney replacement at all – resulting in the death of over 1 million people annually from untreated kidney failure.
Costly facts:
The key to reducing the human and economic costs of CKD and ESKD lies in prevention, for several reasons:
Kidney diseases are silent killers, which can largely affect your quality of life. There are several ways to reduce the risk of developing kidney disease.
This can help to maintain an ideal body weight, reduce your blood pressure and the risk of Chronic Kidney Disease.
The concept On the move for kidney health” is a worldwide collective march involving the public, celebrities and professionals moving across a public area by walking, running and cycling. Why not join them – by whatever means you prefer! Check out the events section of the WKD website for more information.


This can help to maintain an ideal body weight, reduce your blood pressure, prevent diabetes, heart disease and other conditions associated with Chronic Kidney Disease.
Reduce your salt intake. The recommended sodium intake is 5-6 grams of salt per day. This includes the salt already in your foods. (around a teaspoon). To reduce your salt intake, try and limit the amount of processed and restaurant food and do not add salt to food. It will be easier to control your salt intake if you prepare the food yourself with fresh ingredients. .
About half of people who have diabetes do not know they have diabetes. Therefore, you need to check your blood sugar level as part of your general body checkup. This is especially important for those who are approaching middle age or older. About half of people who have diabetes develop kidney damage; but this can be prevented/ limited if the diabetes is well controlled. Check your kidney function regularly with blood and urine tests.


About half of people who have high blood pressure do not know they have high blood pressure. Therefore, you need to check your blood pressure as part of your general body checkup. This is especially important for those who are approaching middle age or older. High blood pressure can damage your kidneys. This is especially likely when associated with other factors like diabetes, high cholesterol and Cardio-Vascular Diseases. The risk can be reduced with good control of blood pressure.
Normal adult blood pressure level is 120/80. Hypertension is diagnosed if, when measured on two different days, the systolic blood pressure readings on both days is ≥140 mmHg and/or the diastolic blood pressure readings on both days is ≥90 mmHg (WHO).
If your blood pressure is persistently elevated above the normal range (especially if you are a young person), you should consult your doctor to discuss the risks, the need for lifestyle modification and medication treatment.
The American Heart Association and the American College of Cardiology revised the guidelines for high blood pressure (2017) and suggested that high blood pressure should be treated earlier with lifestyle changes and medication at 130/80 mm Hg rather than 140/90 mm Hg. However, not all health organizations around the world have adopted this recommendation. Best to consult your doctor.
The right level of fluid intake for any individual depends on many factors including exercise, climate, health conditions, pregnancy and breastfeeding.
Normally this means 8 cups, approximately 2 liters (quarts) per day for a healthy person in a comfortable climate condition.
This needs to be adjusted when in severe climate condition. Your fluid intake may need to be adjusted if you have kidney or heart or liver disease. Consult your doctor on the appropriate fluid intake for your condition.

Smoking slows the flow of blood to the kidneys. When less blood reaches the kidneys, it can decrease their ability to function normally. Smoking also increases the risk of kidney cancer by about 50 per cent.
Common drugs such as non-steroidal anti-inflammatory (NSAIDS)/ pain-killer (e.g. drugs like ibuprofen) can harm the kidneys if taken regularly.
If you have kidney disease or decreased kidney function, taking just a few doses can do harm to your kidneys. If in doubt, check with your doctor or pharmacist.


Certain conditions like diabetes or hypertension are linked to kidney disease, which can be more common in specific populations. Dive into our in-depth discussion on kidney health below to discover valuable insights and help you maintain optimal kidney health.
Chronic Kidney Disease (CKD) disproportionately affects disadvantaged populations, due to hampered healthcare pathways that span from limited access to treatment to poor healthcare outcomes. This has major public health implications due to the devastating impact of kidney failure and the extremely high cost of kidney replacement therapy (KRT).

Due to ethnicity, socioeconomic status and living conditions, some communities face a heightened risk of CKD. For example, African, American Indian, Hispanic, Asian and Aboriginal populations are known to suffer from higher rates of diabetes and high blood pressure, which are leading causes of CKD.
In the US:
In Australia:
In Canada:
Lower socioeconomic status elevates the risk of CKD, irrespective of ethnicity. Language barriers, low education and literacy levels, low income, unemployment, lack of adequate health insurance, and certain culture-specific health beliefs pose barriers to disease prevention and treatment.
There are also stark global imbalances as resource-poor nations face limited access to kidney care. Transplantation is rare in most Low Middle Income Countries, due to a lack of infrastructure and the cost of immunosuppressive drugs, malnutrition and infectious diseases posing life-threatening risks. For example, kidney replacement therapy (KRT) is accessible to less than 10% of Indian End Stage Kidney Disease (ESKD) patients while up to 70% of those starting dialysis die or stop treatment, due to cost, within the first 3 months. Approximately 80% of the world’s KRT patients live in Europe, Japan or North America.
Acute Kidney Injury (AKI) is the rapid loss of kidney function over a few days or even hours.
This sudden decline in kidney performance can result from various causes, including reduced blood flow to the kidneys or exposure to toxins.
Fortunately, the kidneys can often recover almost fully with prompt treatment. Immediate interventions may include fluid and mineral replacement, and in some cases, dialysis may be necessary.
To prevent complete kidney failure, greater awareness of AKI is crucial, especially among those with risk factors. Early detection and intervention are key to improving outcomes.
Acute kidney injury has three main causes:
You have a greater chance of getting acute kidney injury if:
Symptoms of acute kidney injury may include:
Some people may not exhibit any symptoms. For those who are already severely ill, the underlying condition causing AKI might also be producing other symptoms.
In the developed world, AKI is often seen in hospital settings. U.S. data suggests that 5% to 20% of critically ill patients in intensive care units experience an episode of AKI during the course of their illness, significantly worsening outcomes. Increased awareness of AKI among all healthcare workers is essential. Preventive measures, such as careful management of prescription medications in elderly patients, are particularly important.
In the developing world, AKI often results from infections and severe dehydration, such as from gastroenteritis and malaria. Additionally, victims of crush injuries in natural disasters like earthquakes frequently die of AKI. Many cases of AKI in these regions can be prevented through community education and training local workers to recognize early warning signs and implement immediate interventions.
Most organs in our body have strong links and interdependency. Heart and kidneys are not an exception. There is a strong connection between kidney disease and cardiovascular (heart and blood vessels) disease. People with CKD are known to have an increased risk of a stroke or heart at a younger age, because of changes in the circulation caused by kidney disease.

Cardiovascular diseases (CVDs) are a group of disorders of the heart and blood vessels. Any problem that keeps the heart from pumping blood as it should can be classified as CVD.
Cardiovascular diseases include:
Kidney Disease and Cardiovascular Disease are closely intertwined, as many of our body’s organs depend on each other. People with CKD are known to have an increased risk of a stroke or heart attack at a younger age because of changes in the blood circulation resulting from kidney disease.
Shared risk factors for both heart and kidney diseases include:
While it’s not always possible to prevent kidney and heart diseases, certain steps can reduce the risk of adopting one such as
Diabetes is the leading cause of kidney failure. In many countries, half of all people starting dialysis have kidney failure caused by diabetes.

Diabetes is a chronic, metabolic disease characterized by heightened blood glucose levels, causing gradual and severe damage to the heart, blood vessels, eyes, kidneys, and nerves.
Many people with diabetes also develop high blood pressure. High blood pressure and diabetes are considered the leading causes of kidney disease, with diabetes being the leading cause of kidney failure. In many countries, half of all people starting dialysis have kidney failure caused by diabetes.
When diabetes is uncontrolled, high blood sugar damages the tiny blood vessels in the kidneys and alters filtration by the kidneys. This causes Chronic Kidney Disease called Diabetic Nephropathy or diabetic kidney disease.
In most cases, diabetic kidney disease does not manifest itself with any symptoms. The only way to diagnose it is to do blood and urine tests.
The first sign of this damage is finding albumin in the urine. This can be detected by a urine strip test, often called a dipstick. If there is albumin in the urine, an eGFR blood test is also needed.
You should get tested every year for kidney disease if you:
1) Have type 2 diabetes.
2) Have had type 1 diabetes for more than five years.
You are at higher risk of diabetic kidney disease if you :
It is important to note that African Americans, American Indians, and Hispanics/Latinos develop diabetes, kidney disease, and kidney failure at a higher rate than Caucasians.
The best way to slow or prevent diabetes-related kidney disease is by achieving and maintaining target blood glucose and blood pressure levels. This can be achieved through healthy lifestyle practices and taking medicines as prescribed.
Find out more:
Hypertension is the medical term for high blood pressure. For most people, a blood pressure of 140/90 mmHg or higher is considered abnormal.
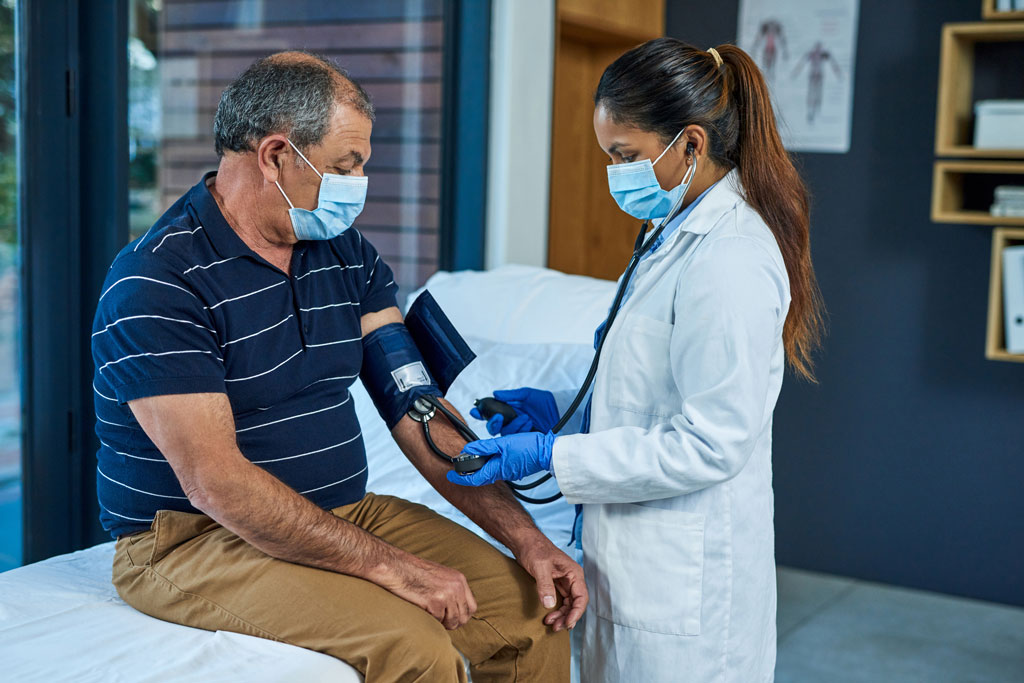
Hypertension, commonly known as high blood pressure, is a condition where the force of the blood against the walls of the arteries is consistently too high.
A typical blood pressure reading is written as two numbers, such as 120/80 mmHg. The first number (systolic pressure) measures the pressure in your arteries when your heart beats, and the second number (diastolic pressure) measures the pressure in your arteries when your heart rests between beats.
For most people, a blood pressure of 120/80 mmHg is considered normal. Hypertension is typically defined as a blood pressure of 140/90 mmHg or higher.
Hypertension is a leading cause of chronic kidney disease (CKD). High blood pressure can damage the blood vessels in the kidneys, impairing their ability to function properly. When these vessels are damaged, the kidneys may fail to remove waste and excess fluid from the body effectively. This excess fluid can further increase blood pressure, creating a dangerous cycle.
Conversely, kidney disease can also lead to high blood pressure, which in turn accelerates kidney deterioration. Approximately 90% of individuals with CKD stages 3-5 have hypertension.
Hypertension often has no initial symptoms but can lead to long-term complications, including damage to the heart, eyes, and kidneys. This damage can occur gradually over many years without noticeable symptoms. However, some patients with hypertension may experience headaches.
Similarly, kidney disease typically does not often present symptoms in its early stages.
Managing blood pressure with medication and lifestyle changes helps to protect the kidneys from further damage. This is why it is instrumental for people with high blood pressure to get tested for kidney disease.
Lifestyle changes include:
Find out more at:
High Blood Pressure and Kidney Disease – National Institutes of Health
While kidney disease affects individuals of all ages and backgrounds, women tend to face unique challenges. With approximately 195 million women worldwide grappling with Chronic Kidney Disease (CKD), it stands as the eighth leading cause of death for women, claiming 600,000 lives annually.

Pyelonephritis (Kidney infection)
Due to their anatomy women are more likely to get urinary tract infections (UTIs) than men. Pyelonephritis is a type of UTI originating from the lower urinary tract and moving upstream to one or both kidneys. Left untreated, such infections can progress to sepsis, presenting life-threatening consequences.
Conception
Advanced-stage CKD, especially when dialysis is required, poses a risk for fertility. Despite the challenges, intensive treatment sessions can make conception on dialysis possible.
Pregnancy-related complications
Access to healthcare
Find out about World Kidney Day and the Taskforce on Women and Non-Communicable Disease position on “Kidney Disease in Women. A Call to Action”, offering evidence-based insights and policy recommendations. It was published in 2018, marking World Kidney Day’s theme “Women & Kidney Disease”.
Read a Scientific Editorial written on World Kidney Day 2018, underscoring the importance of addressing gender-specific challenges.
Being overweight may increase the risk of developing a number of health issues, including diabetes, cardiovascular disease, hypertension, kidney disease and more.
It is estimated that by 2025, obesity will affect 18% of men and 21% of women worldwide. In some nations, obesity is already present in over one-third of the adult population, and overweight in an additional one-third of the population.
Across the globe, obesity is increasing in children, contributing significantly to overall poor health and high annual medical costs.

Overweight and obesity, as defined by the World Health Organization (WHO), is the “abnormal or excessive fat accumulation that may impair health”. Often the definition of obesity is based on the Body Mass Index (BMI) which is measured by dividing weight in kilograms by height in meters squared (kg/m2).
According to the WHO, BMI is classified as:
Note: Different cutoff points are applied for children and adults.
Individuals with obesity, including those with diabetes and hypertension, face an elevated risk of kidney disease. Obesity may lead to CKD indirectly by increasing type 2 diabetes, hypertension and heart disease, and also by causing direct kidney damage by increasing the workload of the kidneys and other mechanisms.
The risk of developing End Stage Kidney Disease (ESKD) for overweight or obese individuals is 2 to 7 times higher in comparison to those of normal weight. People suffering from obesity are also at a higher risk of Acute Kidney Injury (AKI).
In most cases, obesity is preventable and treatable through lifestyle changes. For overweight people, losing as little as 5% of body weight may lower the risk for several diseases. Slow and steady weight loss of half to one kilogram (1 to 2 pounds) per week, and not more than 1.5 kilograms (3 pounds) per week, is recommended as the safest way to lose weight. However, sometimes, the patient may require medical assistance to lose weight.
Here are some examples of actions to help lose weight safely and healthily, when possible:
In 2017, World Kidney Day’s theme was “Kidney Disease & Obesity” emphasizing the critical link between the two. Explore the joint position document by World Kidney Day and the World Obesity Federation, summarizing some key data on the relation between obesity and kidney disease, along with recommended policies and strategies for governments and policymakers.
Organ donation occurs when a person consents to have their organs removed for transplantation, either while they are alive or, if deceased, with the consent of their next of kin. Donations can come from living donors or from those who have passed away.
There are two types of donors: living donors and deceased donors.
Living donors are healthy individuals who voluntarily choose to donate an organ. Typically, living donors are over 18 years old and undergo extensive mental and physical health assessments to ensure they fully understand the risks and implications of donation. Regulations for living organ donation vary slightly from country to country.
Deceased donors are individuals who have passed away and previously expressed their wish to donate their organs. Whilst many people register as potential deceased donors, only some are suitable candidates. Deceased donors must be declared brain dead, often due to conditions like brain aneurysms, strokes, or severe head trauma.
Every organ donation is a gift of life for someone in need.
Living donors can donate organs or parts of organs, such as a kidney or a portion of their liver or lung, as well as tissues, blood, and bone marrow. However, most organ donations come from deceased donors.
Deceased donors can save up to eight lives, as they can donate one heart, two lungs, one liver, one pancreas, two kidneys, and intestines.
The procedures and policies for matching donors with patients vary by country, but the physiological requirements are consistent. Factors typically considered include:
Distance is also considered in some cases, as some organs cannot survive outside the body for more than a few hours. For example, kidneys can be stored outside the body for up to 30 hours.
Most living donations are from family members due to the higher likelihood of a biological match. However, advances in immunosuppressant medications have made it possible for donors and recipients not to be blood relatives. There has also been an increase in altruistic donors and paired donations.
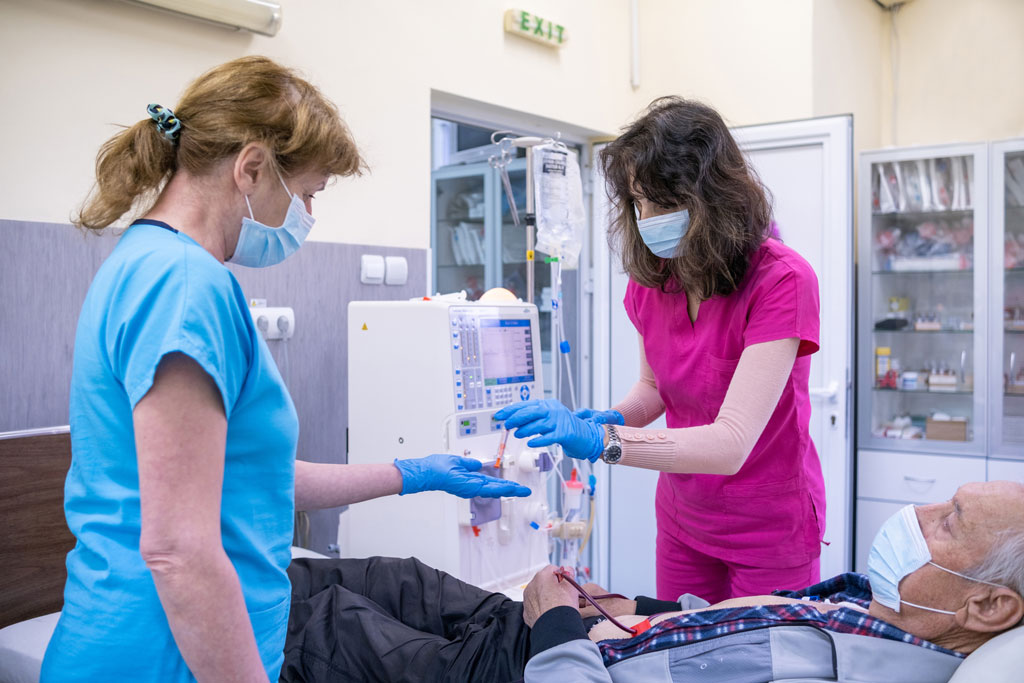
Healthy kidneys clean blood and remove extra fluid in the form of urine. They also make substances that keep the body healthy. Dialysis – both in the center and at home – replaces the blood cleaning functions when kidneys no longer work.
There are two types of dialysis: hemodialysis (HD) and peritoneal dialysis (PD).
In hemodialysis (HD), blood is pumped through a dialysis machine to remove waste products and excess fluids. This process can be done at an in-center (iHD) or at home (HHD). In-center sessions typically take place three times a week lasting three to five hours. At home, the procedure is performed three to seven times per week and takes between three and ten hours per session, often during sleep.
Peritoneal dialysis (PD) works on the same principle as hemodialysis, but blood is cleaned inside the body rather than in a machine. A treatment solution is introduced into the abdomen letting it remove waste products from the blood and then draining it out. It is typically done at home. Some patients can perform peritoneal dialysis continuously while going about normal daily activities or at night using a peritoneal dialysis machine—also called a cycler.
Half a century ago transplantation was regarded as an experimental, high-risk procedure with limited potential. Fast forward to today, it has become a routine clinical practice in over 80 countries.
In terms of improving the patient’s quality of life and cost-effectiveness kidney transplantation is widely regarded as the best option among Kidney Replacement Therapy (KRT) procedures, which also includes dialysis.
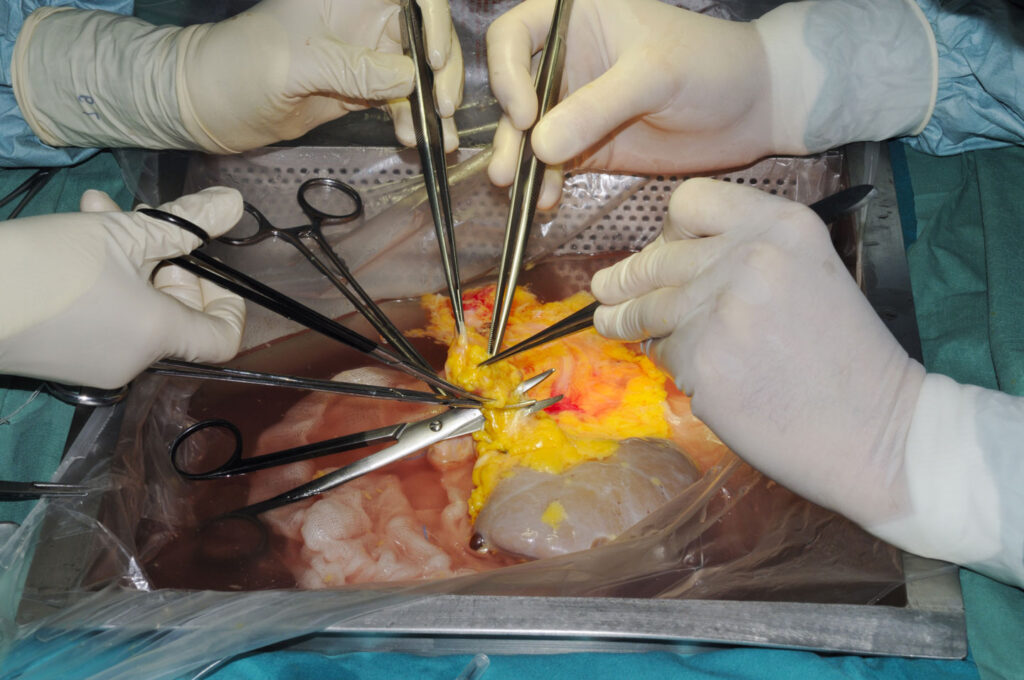
A kidney transplant is a surgical procedure to place a healthy kidney from a donor into a recipient whose diseased kidneys can no longer function adequately. Only one healthy kidney is needed for survival.
Kidney transplantation is considered the best treatment for individuals with severe chronic kidney disease (CKD) or end-stage kidney disease (ESKD), as it significantly improves quality of life and survival rates compared to dialysis.
Kidneys for transplantation can come from a living family member, a living non-relative, or from individuals who have died and donated their organs (also known as cadaver donors).
Overall, the success rates for kidney transplants are high. Living donor transplants have a 90 to 95% success rate. Transplants from deceased donors have 85 to 90% success rate for the first year. Long-term success rates are positive across all age groups.
The kidney transplant surgery is performed in an operating room under general anesthesia. During the operation, a kidney from either a living or deceased donor is transplanted into the recipient. Remarkably, the transplanted kidney typically starts functioning within hours after the surgery.
If there are no complications, patients usually spend up to five days in the hospital and then have an eight-week recovery period at home, during which they gradually resume their normal activities.
For successful functioning of the transplanted kidney, patients need to:
According to the World Health Organization, kidney transplantation is by far the most frequently performed transplant globally. It was the first organ to be ever transplanted. Back in December 1945, Joseph Murray performed kidney transplantation between identical twins. This operation marked a new era for patients with End-Stage Kidney Disease (ESKD).
Since then the number of successfully performed kidney transplants continues to rise annually. In 2015 alone, over 84,000 kidney transplantations were performed worldwide, showing a 5.5% increase from 2014, according to the report from the Global Observatory on Donation and Transplantation.
Explore the global distribution of kidney transplants below: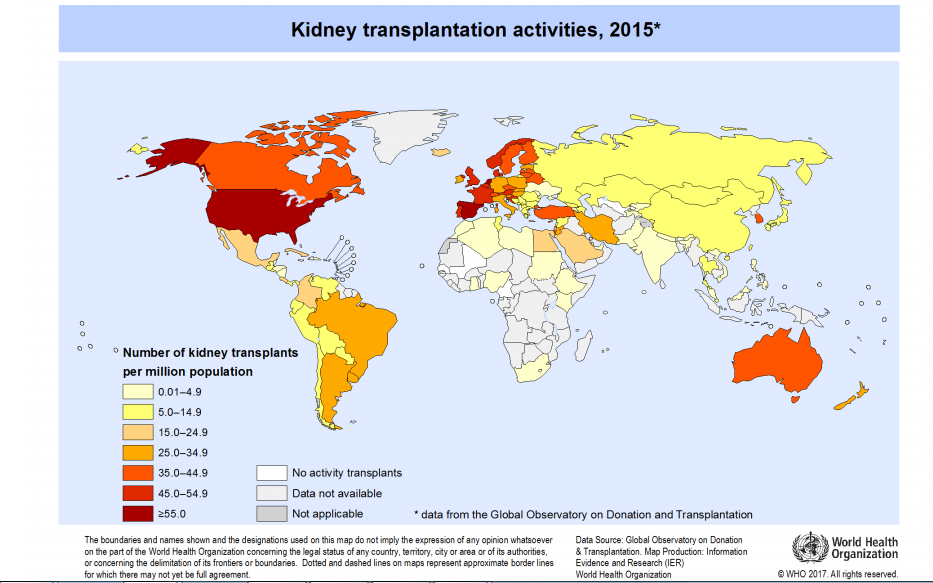
There has been a shortage of donated kidneys leading to long waiting lists for potential transplant recipients. For example, in the United States over 41,000 organs were donated in 2016 but the national waiting list in 2017 was over twice as long, exceeding 116 000 patients, according to U.S. Government data.
This growing gap has given rise to several challenges and ethical concerns in organ transplantation, including organ trafficking, transplant commercialism, and transplant tourism.
Therefore World Kidney Day supports The Declaration of Istanbul, which suggests that “organs for transplantation should be equitably allocated within countries or jurisdictions to suitable recipients without regard to gender, ethnicity, religion, or social or financial status”.
To acknowledge the well-being of living kidney donors and to advocate for promoting this life-saving procedure. The Transplantation Society and the International Society of Nephrology jointly adopted a consensus statement. Both living and deceased donor donations are critical for nations to develop self-sufficiency for organ transplantation.
World Kidney Day is firmly against organ trafficking or transplant tourism of any kind!
World Kidney Day (WKD) in 2012 was devoted to spreading the message of the importance of organ donation and kidney transplantation for people with ESKD.
To find out more about these possible treatments and how they work, visit https://www.uptodate.com/contents/dialysis-or-kidney-transplantation-which-is-right-for-me-beyond-the-basics
Find out more:


World Kidney Day
ISN – Global Operations Center
Avenue des Arts 1-2, 6th floor,
1210, Brussels, Belgium
Tel +32 2 808 04 20
info@worldkidneyday.org